Foreign body aspiration (FBA), although more frequent in children,1–3 is a potentially life-threatening emergency3–7 that can occur at any age.5 Patients may be asymptomatic, have a choking event,6 cough attacks with inspiratory stridor,3 or symptoms may vary3,8 from trivial or chronic nonspecific symptoms8 (dyspnea,9 cough,3 sputum, wheezing3,9) and mimic other lung diseases.8 Hence, in sub-acute and chronic respiratory infections, pulmonary abscesses, haemoptysis, asthmatiform syndrome, localized bronchiectasis or when a lung neoplasia is suspected FBA must be considered.10,11
Although it has little diagnostic value (sensitivity of 28–60%; specificity of 68%),4,7 chest radiography (CXR) is the initial test for FBA.4
Unless patients remember an aspiration event, diagnosis of FBA can be delayed for months even years,1,3 which increases the rate of complications.3,5 When FBA is suspected, a bronchoscopy must be performed to remove the FB (foreign body).9
In order to evaluate the role of bronchoscopy in FBA, we retrospectively collected data of all suspected FBA that were treated by bronchoscopy in our unit from November 2008 to October 2015 and analyzed those performed in adults aged over 18 years-old.
A total of 135 bronchoscopies for FBA suspicion were performed, 69 (51.1%) in adults. The majority of adult patients were male (n=44; 63.8%) and had a mean age of 63±17 years-old. In 12 (17.3%) cases, clinical manifestations were unavailable since patients were referred to our unit from another hospital. The remaining patients reported a choking episode (n=34; 49.3%), pneumonia (n=10; 14.5%), dyspnea (n=4; 5.8%), trauma (n=3; 4.3%) or a cardio-respiratory arrest (n=1; 1.4%). Five patients (7.2%) were asymptomatic. Mean time between aspiration and bronchoscopy was 77.7±173.1h (not known/available in 36 cases). In the 53 cases (76.8%) with an available CXR, 33 (62.3%) were abnormal, in which a condensation (n=13), atelectasis (n=10), visible FB (n=9) or hyperinflation (n=1) was identified.
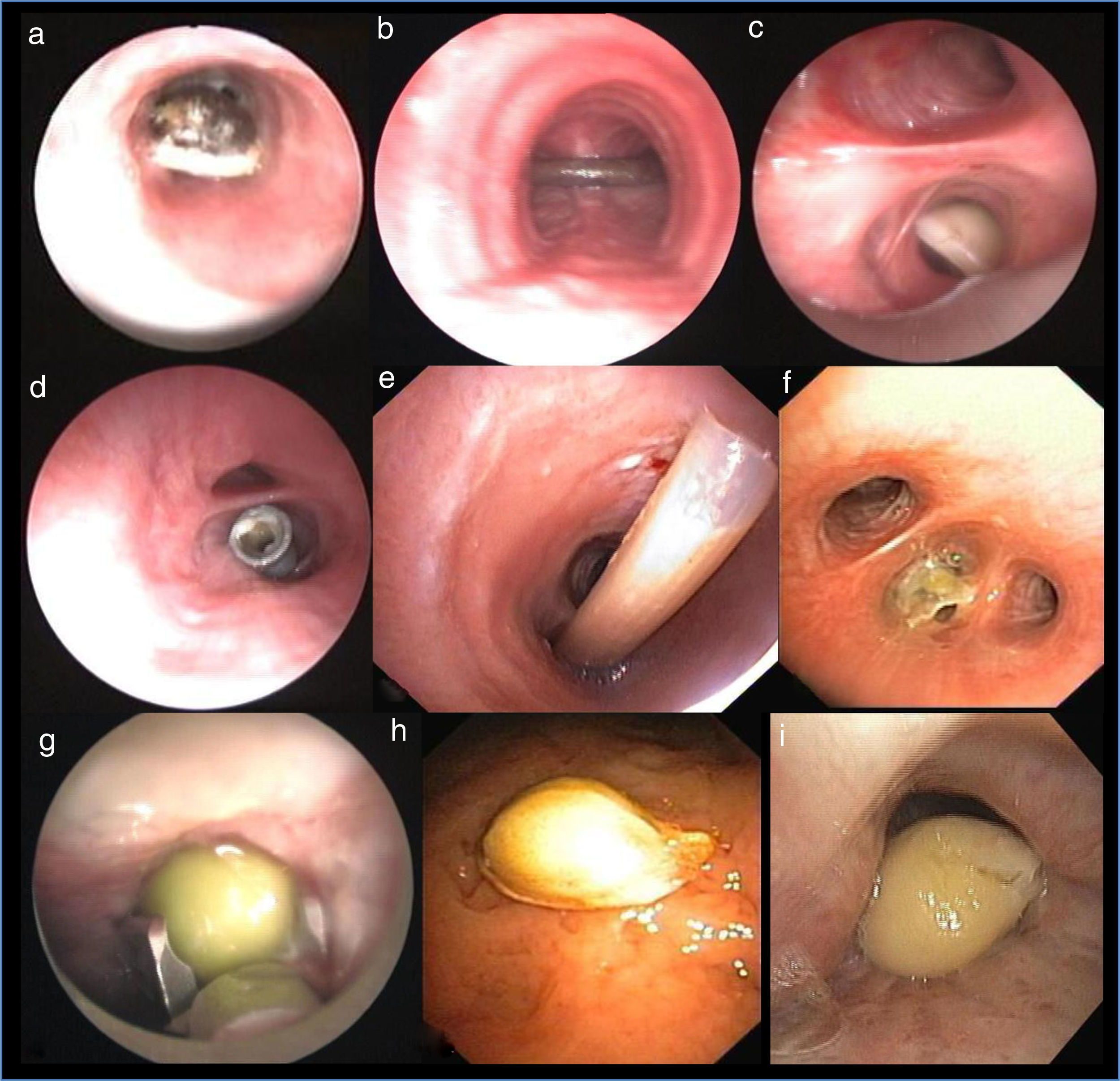
A rigid bronchoscopy was performed in 40 patients (58%) and a flexible bronchoscopy in 29 (42%). A FB was seen and removed in 53 (76.8%) patients (Table 1). We removed bones (n=9; 17%), dentistry material (n=7; 13.2%), tracheostomy material (n=6; 11.3%), plastic objects (n=5; 9.4%), beans (n=5; 9.4%), other organic food (n=5; 9.4%), pills (n=4; 7.5%), seeds (n=4; 7.5%), meat (n=3; 5.7%), nuts (n=2; 3.8%), teeth (n=2; 3.8%) and one (1.9%) unidentified metallic object (Fig. 1). Five FBA occurred during a dental procedure and two after facial trauma.
Crosstabulation between type of bronchoscopy used and visualization of foreign body and between chest X-ray and visualization of foreign body.
| Airway foreign body | Total | ||||||
|---|---|---|---|---|---|---|---|
| Present | Absent | N | % | ||||
| N | % | N | % | ||||
| Bronchoscopy used | Rigid | 36 | 52.2 | 4 | 5.8 | 40 | 58 |
| Flexible | 17 | 24.6 | 12 | 17.4 | 29 | 42 | |
| Result of chest X-ray | Abnormal | 27 | 50.9 | 6 | 11.3 | 33 | 62.2 |
| Normal | 12 | 22.6 | 8 | 15.1 | 20 | 37.7 | |
Endobronchial pictures of some foreign bodies found: (a) sunflower seed in the right main bronchus; (b) plastic tube over the carina; (c) tooth in the right lower lobar bronchus; (d) metallic piece in the medial segment of the right middle lobar bronchus; (e) plastic tube in the trachea and left main bronchus; (f) plastic piece in right lower lobar bronchus; (g) pea in the right upper lobar bronchus; (h) orange seed in the right middle lobar bronchus; (i) chickpea in the right main bronchus.
Clinical symptoms and FB presence were discordant in 19 (35.2%) patients (14 symptomatic without FB; five asymptomatic with FB). CXR and FB presence were discordant in 18 (33.9%) cases (Table 1). CXR sensitivity was 69.2%, with 57.1% of specificity, 81.8% of positive predictive value, 40% of negative predictive, likelihood ratio for positive results of 1.61 and likelihood ratio for negative results of 0.53.
FB were found in the right bronchial tree (n=32; 60.4%), left bronchial tree (n=13; 24.5%), trachea (n=5; 9.4%) and vocal folds (n=1; 1.9%). In two cases (3.8%), FB were found in both sides. There were no major technique complications or need for surgery referral.
FBA has been described to be more frequent in children than in adults,1–3 although we performed more bronchoscopies for FBA suspicion in adults. We also performed more bronchoscopies per year for FBA than described in other series.2,5,8,11 This high rate could be explained by the fact that our hospital has a dedicated bronchologist available on call 24h a day/7 days a week, and is the center of reference of Lisbon and south of Portugal in cases of FBA.
When FBA is suspected, a rigid or flexible bronchoscopy can be performed, and debate remains which one is the optimal procedure.1 Many bronchologists consider rigid bronchoscopy as the treatment of choice,6,9,10 since it is extremely effective10 and has a low complication risk.9,10 In our unit, we prefer to performed a rigid bronchoscopy for FB extraction followed by a flexible bronchoscopy to ensure the absence of another FB lodged more distally.
A normal history and/or CXR is not uncommon in suspected FBA.7 In fact, we found a discordance of 27.5% between clinical symptoms and the presence of FB and 33.9% between CXR and the presence of FB. In our study, CXR had a low diagnostic accuracy, as a low positive likelihood ratio was found.
Since it is difficult to correctly diagnose FBA without a bronchoscopy, a negative bronchoscopy rate of 25–47% is expected.7 In our study, 23% of the bronchoscopies were negative.
As in other series,2,11,12 the majority of FB were found in the right bronchial tree, which can be explained by the vertical nature of the right main bronchus, its larger diameter, the greater airflow through it, and the localization of the carina to the left of the midline of the trachea.12
In conclusion, FBA in adults is not rare in adults and, even if there are no clinical or radiological findings, a bronchoscopy should always be performed.
FundingThis article did not receive any grant or other support.
Conflicts of interestThe authors have no conflicts of interest to declare.