Multiple system atrophy (MSA) is a rapidly progressive adult neurodegenerative disease associated with sleep disorders, such as rapid eye movement (REM) sleep behavior disorder (RBD), obstructive sleep apnea syndrome (OSAS), or stridor.1,2
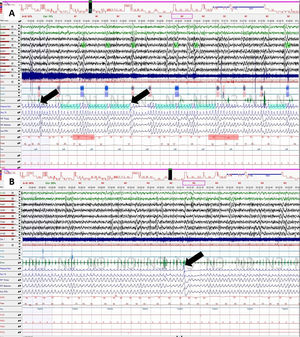
A 63-year-old hypertensive woman with sleep onset insomnia complained of harmful motor activity and vivid dreams. The patient had no history of snoring, or other night symptoms, or complaints related to excessive daytime sleepiness. Epworth sleepiness scale score was of 6. She underwent polysomnography which revealed micro-arousal index of 42.4%, respiratory disturbance index of 18.9/h, periodic limb movements (PLM) of 67.5/h, frequent gesticulation and somniloquism and REM sleep without atonia. OSAS plus PLM syndrome and RBD were diagnosed, and she started continuous positive airway pressure treatment and clonazepam 0.5 mg/id. A year later she complained of multiple falls and orthostatic hypotension. Neurological examination revealed scanning dysarthria, distal polyminimyoclonus, limb dysmetria and ataxia A cerebellar-type probable MSA was diagnosed and the patient started levodopa/carbidopa 25/100 mg 3id partially improving symptoms. The polysomnography was reassessed and concluded the existence of multiple inspiratory sighs in different phases of NREM sleep (Fig. 1), a year prior the onset of neurological symptoms.
This typical but barely known polysomnographic respiratory finding in MSA – inspiratory sighs – can be present in short disease duration and could help the differential diagnosis. Specially in the presence of stridor, sighs may increase the likelihood of MSA.3 Besides inspiratory sighs, our patient's polysomnography helps the diagnosis of OSAS, PLM syndrome, and RBD. These are common both in MSA and in Parkinson's disease, and usually start before neurological complaints.2
In conclusion, pulmonologists in sleep medicine should be aware of this polysomnographic picture (inspiratory sighs, OSAS, PLM syndrome, and RBD) since it could point towards the presence of an extrapyramidal disease, including MSA. Careful evaluation of polysomnography may help to identify early signs of these neurodegenerative diseases and lead to early referral for a neurological consultation.
Declaration of Competing InterestThe authors have no conflicts of interest to declare.
Source of fundingThis research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.